New layers in research, treatment of sickle cell trait and stroke
By American Heart Association News
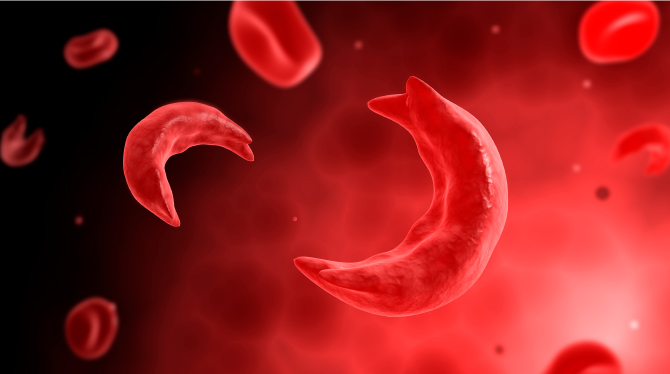
Sickle cell disease increases the risk of stroke for African Americans – but recent research shows carrying the genetic trait for sickle cell doesn’t.
It’s a new layer on the study and treatment of these inherited conditions affecting red blood cells, and experts say it should prompt doctors to dig deeper.
Past studies have suggested there may be a link between stroke and the two conditions. Others have shown none. Some research also has associated the sickle cell trait with chronic kidney disease, and lung and deep vein blood clots, all of which are potential risk factors for stroke.
But Dr. Hyacinth I. Hyacinth, who led the recent study that found no link between the trait and stroke among African Americans, said the bottom line is medical professionals may need to spend more time and effort treating stroke victims who have sickle cell trait.
The research “tells neurologists that in the scenario where a patient with sickle cell trait presents with stroke and no apparent traditional risk factor, a more thorough work-up should be done instead of just pinning the stroke on the fact that the patient has sickle cell trait,” said Hyacinth, assistant professor of pediatric hematology-oncology at Emory University School of Medicine in Atlanta.
Sickle cell disease has been a well-established risk factor for stroke. In the disease, crescent-shaped or "sickled" red blood cells are less able to carry oxygen to the body's tissues and organs. These cells can stick to vessel walls, which can block arteries to the brain and cause a stroke. But with sickle cell trait, a person has inherited one sickle cell gene and one normal gene. They usually have no symptoms of the disease and can have both regular and sickle-shaped blood cells.
About 1,000 babies are born with sickle cell disease each year, according to the Sickle Cell Disease Association of America. About 70,000 to 100,000 people in the United States have sickle cell disease and 3 million have sickle cell trait.
Globally, it affects millions. The United Nations designated Tuesday as World Sickle Cell Day.
The study Hyacinth led, published in JAMA Neurology(link opens in new window), included data from 19,464 people with an average age of 60 to see how sickle cell trait impacted the risk of ischemic stroke, the most common form of stroke. The data included 1,520 people with sickle cell trait, and 620 people with stroke.
Dr. Olajide Williams, chief of staff of neurology at Columbia University, agreed doctors need to keep investigating when it comes to treating African American patients.
“Sickle cell trait does not explain the black-white disparities in stroke incidence rates," Williams said. "And its presence should not detract from the need to (search) for other medical causes in a stroke patient.”
He said the recent study was limited by the fact that about 48 percent of the sample was not directly genotyped, which could lead to a risk of misclassifying people with sickle cell trait.
“We need studies evaluating the association between sickle cell trait and stroke subtypes,” Williams said. “And more work is needed to understand the observed disparity favoring whites in age-adjusted stroke incidence rates between blacks and whites.”
Hyacinth agreed more in-depth studies are needed, but he said the overall message of the new study is clear: “If you or someone with sickle cell trait has a stroke, it is very unlikely that sickle cell trait is the only risk factor.”
If you have questions or comments about this story, please email [email protected].




